Mental health problems accumulate and result from many factors – globalisation, social and economic conditions, difficulties related to adolescence, family life issues (divorce or family break-up) as well as relations with parents which – when limited – may cause the feeling of loneliness and auto-destructive behaviours in children. In Poland, 9% of children and young people below 18 years of age (which makes up about 630 thousand) require psychological or psychiatric treatment. In this respect, we do not differ much from other countries where about 10 percent of the population of children and young people need professional help.
The data of the National Police Headquarters reveal that suicides are the second most frequent cause of death among teenagers. At the same time, Poland is in the lead among European countries in terms of the number of suicides. More and more young people are trying to take their lives every year. The number of suicide attempts among minors aged 7-18 grew from 730 in 2017 through 772 in 2018 to as many as 485 in the first half of 2019. From 2017 to the first half of 2019, 250 out of 1987 suicide attempts ended in death. In 585 cases the suicide attempts resulted from a mental illness and in 374 cases from mental disorders.
The primary principle in the therapy of children and young people is the comprehensiveness. The key to success is the psychological and medical diagnosis accompanied by multidisciplinary treatment and rehabilitation process, including the social and family context where the child is functioning.
The NIK audit showed that the system of psychiatric treatment of children and young people does not provide comprehensive and commonly available health care in this area. By the end of the NIK audit, the Minister of Health did not implement the community treatment model for minors with mental disorders. This model assumes that the child should be given support in a friendly environment, ideally in his or her family, at school, or in a psychological and pedagogical counseling centre. Only then ambulatory treatment should be provided, e.g. in a mental health outpatient clinic. And if this solution does not help the minor is to be placed in a hospital. This is the most effective form of treatment of this population. Implementing this treatment model with children and young people as obligatory is a prerequisite for the development of psychiatric treatment.
NIK has stressed that the Minister of Health developed a three-step psychiatric care model but the new solutions started to be implemented after the end of the NIK audit. That is why the model's effectiveness could not be evaluated.
According to NIK the Minister of Health did not define the ratios of a minimum number of psychiatrists for children and young people to satisfy the real needs. Also, no model was developed to predict the demand for psychiatrists so that a required number of them could be provided, also considering the demographic changes. Therefore, it remains unknown how many doctors are needed now and how many will be needed in the future. At the end of March 2019, as many as 419 doctors worked as psychiatrists of children and young people and 169 were in the psychiatry specialty training. The national consultant for children and young people psychiatry indicated a deficit of about 300 psychiatrists. Also, the age structure among medical staff was an adverse factor, as 32% of specialists were over 55 years old. In the coming years, the psychiatrists' deficit issue may get even worse as only a small part of vacancies in psychiatry training provided by the Minister of Health to resident doctors was occupied. Although the Minister entered the psychiatry of children and young people on the list of priority specialties, it did not make doctors much more interested in this specialty. Out of 161 training vacancies in this area, only 39 persons (that is over 24%) resolved to take training in this specialty.
Though, in the opinion of NIK, the biggest problem is the patchy distribution of psychiatrists for children and young people Poland-wide. The smallest number of psychiatrists per 10 thousand minors was in Lubuskie Province (0.16) and the biggest – in Łódzkie Province (0.79). At the same time, there was the smallest number of psychiatrists per 1 thousand minors in Podkarpackie Province (1.02) and the biggest – also in Łódzkie Province (4.96).
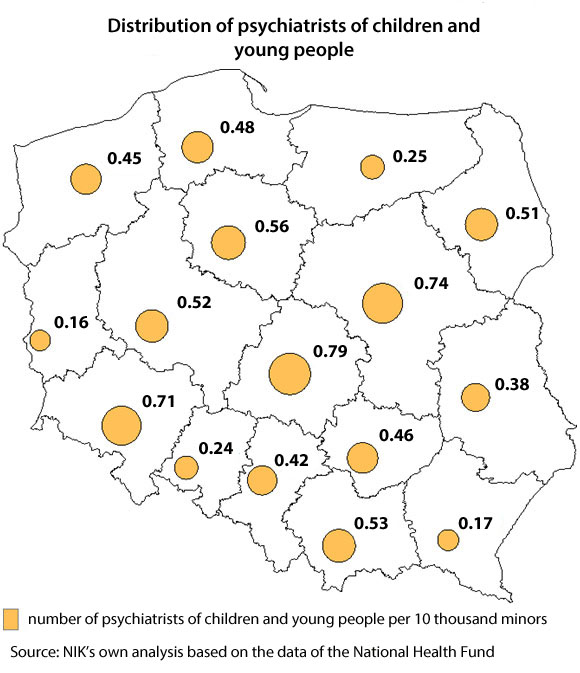
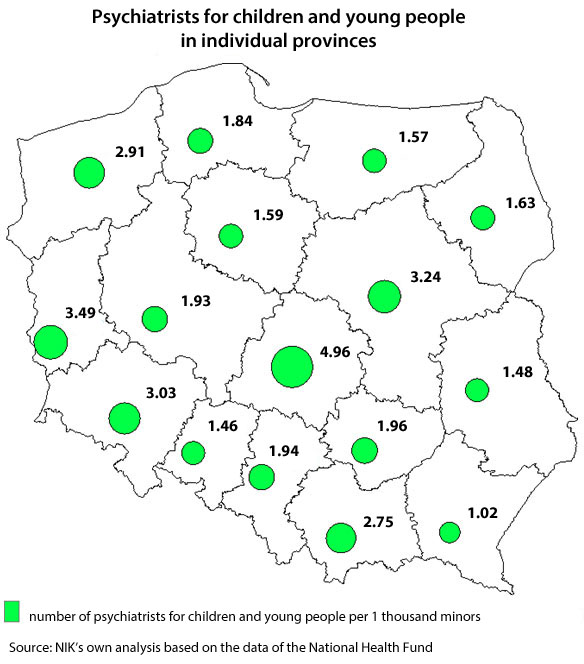
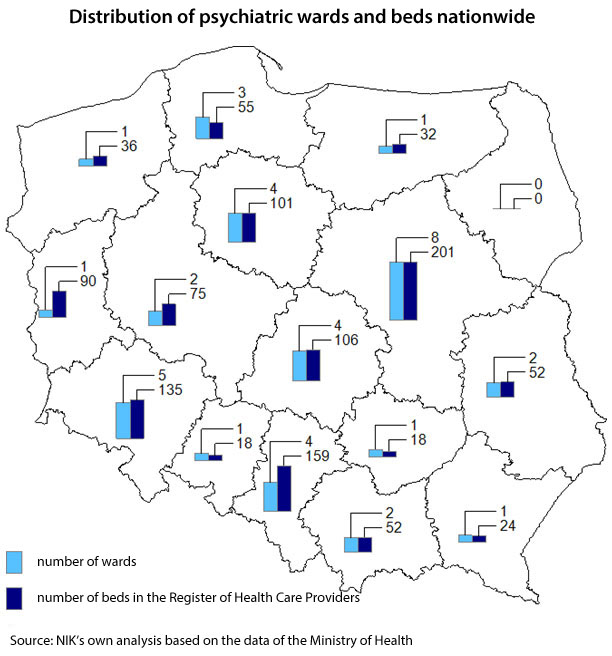
The patchy distribution was also valid for psychiatric hospital wards for children and young people. Not a single psychiatric ward of this type was found in Podlaskie Province and there were no day psychiatric wards in five other provinces: Lubuskie, Opolskie, Świętokrzyskie, Warmińsko - Mazurskie, and Zachodniopomorskie. Nationwide, as of the end of 2018, psychiatric services for children and young people were provided in 36 hospital wards (at the end of the first half of 2019 it was 40).
As many as 402 minor patients in a stable condition waited to be admitted to the psychiatric hospital ward, i.e. 114 fewer persons than in 2017. The average waiting time dropped from 2 days in 2017 to 1.5 days in 2018. From among 8 audited hospitals, as of the end of 2018, patients in a stable health condition waited to be admitted to 3 hospitals for a month, two weeks, and 11 days. Only in one hospital patients in need of urgent hospitalisation waited 13 days on average.
NIK has pointed out that in two hospitals due to the deficit of vacancies minor patients were also placed in adult wards.
In most cases, the minimum headcount levels in psychiatry wards for children and young people were reached or even exceeded. A problem was insufficient financing of the psychiatric treatment of that population. The funds paid to hospitals by the National Health Fund did not cover the patents’ treatment costs.
NIK has underlined inadequate supervision of provincial consultants in psychiatry of children and young people over psychiatric wards. They carried out inspections only in 2 out of 8 hospitals audited by NIK. It should be noted that the national consultant in psychiatry of children and young people did not conduct any inspection in this area.
As for the number of vacancies and the waiting time it was even worse in outpatient clinics. The facilities’ directors reported that considering the high demand for psychiatric treatment of children and young people the number of outpatient clinics is too small and that is the reason why queues in the clinic get longer and longer. The number of patients waiting for psychiatric treatment was going up every year. In 2017, in the audited clinics, it was on average 564 persons, in 2018: 661 persons and in 2019 – 1036 persons. In one outpatient clinic, the average waiting time was as long as 120 days.
The explanation was that the big number of patients waiting for a visit and a long waiting time resulted mainly from the deficit of psychiatrists working with children and young people.
The headcount level in psychiatric outpatient clinics met the minimum norms defined by the law but the number of patients per one FTE in 2017 (1091 on average) increased in 2018 to the average of 1124. In the outpatient clinic in Pisz, there were 593 persons and in Rzeszów, it was as many as 2415 patients per a psychiatrist.
A large problem in the psychiatric care of children and young people is the absence of prevention. In more than half of audited outpatient clinics, there was no prevention of mental disorders in place. The explanation was that preventive measures were already taken by schools (a school pedagogue or psychologist) or psychological and pedagogical counselling centres. Nearly half of the state schools of different types (44 percent) do not hire pedagogues or psychologists as individual employees. In the locations where they are employed, the prevention of mental disorders in school is impaired by a big number of students per one pedagogue or psychologist.
It needs to be mentioned that community care teams did not operate in any of the mental health outpatient clinics (out of 13). The facilities’ heads explained that the National Health Fund does not finance community care for children and the outpatient clinics do not provide home visits in psychiatric health care.
Recommendations
NIK has addressed the following recommendations to the Minister of Health:
- to limit the territorial diversification of access to psychiatric care nationwide;
- to develop a model of predicting demand for specialist doctors;
- to provide equal distribution of training centres and training vacancies;
- to define the ratios of the minimum number of psychiatrists for children and young people.


